General Audiologist
> download Report on European University Education in Audiology (Powerpoint-File)
> download "Audiology in Europe" (pdf-file)
> download "EFAS and the ‘General Audiologist’ Model (Powerpoint-File)
> European University Education in Audiology: EFAS Concertation meeting, Bad Zwischenahn (January 17th/18th, 2008)
Audiology in Europe
The General Audiologist - A proposal for a model training programme in general audiology for Europe. The document has been prepared by a special working group during the period 1999-2001 and adopted by the EFAS General Assembly in Bordeaux September 16, 2001.
Introduction
During the last few decades audiology has developed into a scientific and clinic area which encompasses an extremely broad area of expertise. In addition to medicine and physiology, engineering and physics are basic areas which play an important role as the technical development has been very evident both with regard to equipment for diagnostic procedures and to signal processing and outcome assessment in the field of hearing aids, cochlear implants and other means of technical rehabilitation. Psychology is another area of increasing importance, both with regard to the interplay between auditory function and cognitive abilities and in terms of providing a basic understanding of the handicapexperienced by hearing loss and how this can be ameliorated. The importance of helping the hearing-impaired person not only by a correct diagnosis and a professional provision of technical devices but also with regard to his broader needs as a social being has become very evident. These and many other factors illustrate the need for very broad professional skills in audiology today in order to offer the hearing-impaired person the best possible services, allowing him to remain as a functioning member of the modern socity.
An analysis of hearing health care services currently provided in Europe shows that they are far from sufficient in many respects in most European countries. As the improvement of services for the hearing impaired population in Europe is one of the major goals of the European Federation of Audiology Societies, EFAS, its General Assembly EFAS took the initiative for a working group on “European Audiology Training” in Prague 1997. The working group started its work collecting data (specifications, responsibilities, curricula, etc.) about the different professions presently engaged in audiology in Europe. The survey revealed that the infrastructure of formal education in Audiology in Europe needs further development. This task called for a broader consensus which could not be achieved on a working group basis.
Therefore, EFAS organised a workshop on “European Audiology Training (EAT)”, inviting participants representing the different professional groupings presently being active in Audiology in the European countries. This decision was taken at the EFAS General Assembly Oulu, Finland, in June 1999. The workshop was held at the University of Giessen, Germany, October 11-13, 1999. Thirty-three delegates from fifteen European countries participated in the workshop. The discussions on the possible options for an improvement of audiology in Europe lead the delegates to a consensus regarding a long-term goal of the implementation of a new profession, here to be called "General Audiologist”. This professional is seen as the primary contact person for the hearing impaired individuals, supported by other professional groups already engaged in the provision of audiological services. It is realised that the conditions for establishing training programs according to the model proposed in this document may vary considerably among different countries in Europe, depending on how audiological services are organised within the public health system and by private organisations. This may obviously effect both the time course of implementation and the exact curriculum. However, the model described and the contents of the curriculum presented illustrate the totality of professional competence required to provide good service for hearing-impaired patients and which need to be provided.
At the meeting in Giessen it was decided to develop a specification, including a description of professional skills and the contents of a curriculum for a four year training programme for the General Audiologist. By the end of the Workshop a first draft was ready. Since then it has been circulated to the EFAS members and revised according to comments received from national audiology societies. At the EFAS General Assembly in Bordeaux Sept 16, 2001, it was agreed to accept the proposal in its present shape to be considered as a working model for the long-term development of the profession of General Audiologists in Europe.
The Council of EFAS and the participants of the workshop are aware that the implementation of the General Audiologist (GA)
(1) shall not replace but supplement the services of existing hearing health care providers.
(2) has to be accomplished nationally according to the special situation and needs of the various European countries. This process may well lead to different realisations of the profession in different countries. Either the GA may be developed as a completely new profession, or the GA curriculum may be adopted for one of the professional groups already active in this field to broaden its scope.
(3) has a long term perspective. For many European countries it is unlikely that it will be possible to implement the GA right away, but there is a strong commitment to have the GA implemented on a long term run in the European countries for the sake of the hearing impaired population.
List of participants at Workshop in Giessen, Germany, October 1999:
Stig Arlinger, Sweden
Torborg Arvidsson, Sweden
José Barajas, Spain
Moe Bergman, Israel
René Dauman, France
Gottfried Diller, Germany
Salesa Enrique, Spain
Jan Feenstra, The Netherlands
George Gavalas, Greece
Anton Gros, Slovenia
Minka Hildesheimer, Israel
Kerttu Huttunen, Finland
Jürgen Kiessling, Germany
Martin Kinkel, Germany
Ligija Kise, Latvia
Birger Kollmeier, Germany
Lars Kronlund, Finland
Einar Laukli, Norway
Thomas Lenarz, Germany
Gun-Britt Milioris, Sweden
Siri Økstad, Norway
Agnete Parving, Denmark
Alexandru Pascu, Romania
Anders Ringdahl, Sweden
Tony Sirimanna, UK
Martti Sorri, Finland
Wieslaw Sulkowski, Poland
Wim ten Boske, The Netherlands
Dolores Umapathy, UK
Jagoda Vatovec, Slovenia
Hans Verschuure, The Netherlands
Bo Walter, Denmark
Bert van Zanten, The Netherlands
Definition of Audiology
Audiology in terms of this paper deals with function and dysfunction of the auditory system. The services provided to hearing impaired people deal with
1. Diagnostics
2. Auditory (re)habilitation
3. Communication/communication disorders
4. Prevention
5. Research and teaching
Definition of audiology according to the International Society of Audiology
“Audiology deals with the knowledge, protection and rehabilitation of human hearing, inclusive of the effects of pharmacological and surgical measures, but exclusive of matters relating to the techniques of these measures.“
Purpose of this report
The purpose of this report, based on discussions among representatives of fifteen European countries, is to propose common requirements for a qualified general audiologist as seen in a long-term perspective, and to present a proposal for a model training program for such a profession. By presenting such a curriculum in rather great detail, the great width of the field of audiology is clearly illustrated.
Definition of “General Audiologist (GA)“
Currently many professions contribute to audiology, and the high level of audiological competence is provided by a team of audiological specialist/scientists with different backgrounds (e.g., medical audiologists, physical/technical audiologists, educational audiologists).
The broad level of audiological services, however, shall be provided by generalists who are called General Audiologists (GA) in this report. The GA is seen as a person who can provide qualified and relevant services to hearing impaired people. The profession is interdisciplinary and is based on skills in many different fields.
Pyramid approach
The figure illustrates the idea of the General Audiologist representing the broad approach across the various disciplines that contribute to audiology as a complement to specialists, representing greater depth in a more limited area.
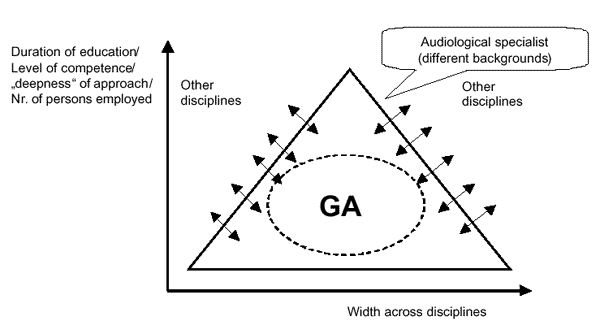
• basic level: General Audiologist (practically oriented),
level: university degree training, (B.Aud, M.Aud)
>> Entrance level: qualification for university/polytechnic
>> 3 years of theoretical studies
>> Practical orientation shown by inclusion of 1 yr practical training
>> GA may migrate to Audiological Specialist by specialisation in an additional field
• high level: Audiological Specialist,
level: university degree (clinically oriented) with specialisation on graduate level:
>> Other professions with specialisation in audiology (medical, physical, educational
degree)
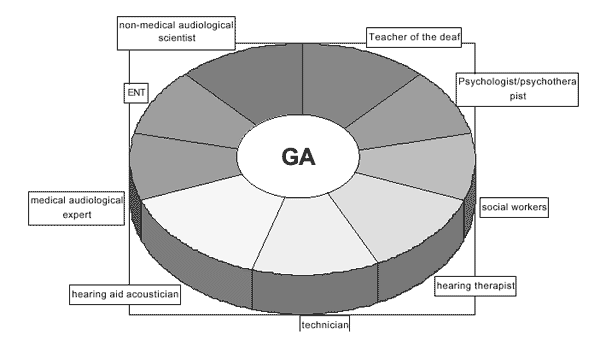
• Related professions such as:
> Teacher for the deaf
> Psychologist/psychotherapist
> Social worker
> Speech and language/hearing therapist
> Technician
> Hearing aid acoustician
> Audiological physician
> Non-medical audiological scientist
> Otorhinolaryngologist
Some can migrate to GA, some can also migrate to Audiological specialist.
Tasks the GA should be able to perform.
The GA should also have sufficient knowledge about the need for referral to those more specialised in these tasks.
• Diagnostics
> Psychoacoustic methods
> Electrophysiological tests
> Acoustic methods
> Paediatric tests
• (Re)habilitation
> Hearing devices
- selection of hearing devices (including assistive listening devices)
- taking ear impressions and making earmold/ITE shell
- fitting including fine tuning of hearing devices
- assessment of fitting outcome/benefit
> Other measures
- communication training (auditory and non-auditory)
- assessment of the communication disability
- screening of the need of alternative and augmentative communication systems
- special requirements of the ageing population
- special requirements of hearing-impaired children (e.g., speech and language
development)
- assessment of acoustic characteristics of listening environment
- management planning after diagnostic assessment
• Educational audiology
• Occupational issues
• Financial matters, compensation issues
• Follow up
> Technical system maintenance
> Training/(re)habilitation
• Counselling (of patients and other professionals)
> Prefit assessment and counselling (including relevant others)
> Social work
> Ethical and cultural issues
> Educational placement of pre- and postlingually hearing-impaired children
> Psychological/psychiatric treatment
• Execution of research in a team (research on humans based on clinical work and using established methods of audiology)
• Assessment of audiological procedures and services
• Counselling of general public
> Awareness
> Prevention
> Health economy issues
> Politics
1. Definition of a curriculum (minimal training requirements)
Proposal for a curriculum:
3 years of theoretical studies:
25% basic sciences, 25% medical and diagnostic audiology, 25% technical and environmental audiology, 25% psychosocial audiology and educational issues, communication repair methods, general skills and specialisation.
1 year of practical studies.
• Basic sciences
> Mathematics
- calculations, statistics
> Physics
- acoustics (incl. room acoustics)
- mechanics
- electronics
> Communication engineering
- basic principles of signal processing
- electronics
- system theory
> Medicine
- general anatomy (basic knowledge)
- anatomy and physiology related to hearing
- embryology
- basic physiology
- pathophysiology (basic knowledge)
> Epidemiology
> Chemistry and Biochemistry
- chemistry of materials
- genetics and molecular biology
- pharmacology
> Speech and hearing sciences
- perception of speech (normal and abnormal)
- phonetics (incl. non-European languages)
- linguistics
- psychoacoustics
- physiological acoustics
> Developmental psychology and education
> Research methodology
- experiment planning
- literature/information retrieval
- ethics in research
• Medical audiology:
> Knowledge of medical conditions associated with hearing and balance (nosological
classification)
- pathophysiology of auditory and vestibular systems
- speech/language acquisition disorders
- malformations
- infections/inflammations
- traumatic hearing disorders
- degenerative diseases
- inheritance
- auto-immune diseases
- tumours
- non-organic hearing impairment
- exposure to loud sounds (industrial, music, leisure time activities)
- toxic agents
> Overview of associated medical disciplines such as
- medical audiology
- geriatrics
- ENT/otorhinolaryngology
- phoniatrics
- anaesthesiology
- imaging techniques
- neurology/neuro-otology/neurosurgery
- paediatrics
- psychiatry
- ophthalmology
- general practice
- genetics
- physiotherapy
> Prevention
- noise induced hearing loss
- ototoxicity
- otitis media
> Other disciplines
- psychology
- information from teachers, nursery staff etc.
• Diagnostical audiology:
> Audiological assessment and site of lesion testing such as
- history
- otoscopy (with appropriate instruments)
- psychoacoustic tests
- electrophysiological tests
- impedance tests
- paediatric tests
- tinnitus evaluation
- others...
> Tests for central hearing disorders
> Basic evaluation of children
- Behavioural Observation Audiometry
- Visual Reinforcement Audiometry
- Conditioned Orientation Reflex audiometry
> Vestibular testing (basic knowledge, related to hearing)
• Technical audiology:
> acoustical measurement and calibration
> electroacoustics: transducers, amplifiers
> signal processing: filters, AGC, etc.
> speech technology
> real ear measurements
> standards
> hearing devices
- hardware/software
- fitting procedures (general and language-dependent)
- outcome/benefit measures
- field tests
- taking ear impressions, making of earmolds
- assistive listening devices
• Environmental audiology
> Noise induced hearing loss
- sources of noises
- sensitivity loss (TTS, PTS)
- individual susceptibility
- interaction of noise and other agents (vibration, chemicals, ageing etc.)
- tinnitus
- acute acoustic trauma
> Extra-auditory effects of noise (basics)
- sources
> Speech interference
- hearing loss
- noise level/spectrum
- reverberation
- language issues (native/non-native, redundancy)
> Management
- current standards for noise exposure
- counselling
- hearing conservation programmes (monitoring of hearing)
- hearing protectors
• Psychosocial audiology and educational issues:
> Linguistics
- phonology
> Phonetics
- speech perception, including second language
> Normal/abnormal speech and language development
- augmentative and alternative communication
> Psychology
- learning theories
- consequences of ageing
- crisis theory
- cognitive development
- emotional development
- psychological aspects of hearing impairment
- psychological aspects of deafness
- coping strategies
> Crisis management
> Psychosocial sequelae of hearing disorders
> Understanding of educational systems and techniques
- special education/pedagogy for children and adults
- educational options available
> Auditory training
- vigilance/detection (awareness of the presence/absence of sounds, continuing attention to a sound)
- discrimination (human voices, environmental sounds, rhythms)
- recognition (environmental sounds, human voices, speech)
- comprehension (smaller and larger speech segments, ideas, contents of messages)
> Speech reading and communication training
- hearing tactics and communication skills
- visual and tactile training
- use of devices
• General professional skills:
> Knowledge of health care system
> Awareness of own professional limitations
> Communication skills (written and oral)
- counselling techniques (patients/relevant others)
- professionals
- team work
- interviewing techniques
> Screening methods for hearing impairment
- neonatal
- other paediatric screening
- occupational health
> Screening for speech and language problems
> Administration
> Project management
> Legislation in health care system
> Social security and compensation issues
> Computing
> Quality management
• Practical work
> Project work
> Thesis work (6 months/minimum 3 months)
> Practical work with patients (minimum 6 months)